I recently did a post-surgery ultrasound to check to see if my body went back to normal after my surgery in September (due to missed miscarriage). I’ve had so many ultrasounds over the years that I’ve learned to spot abnormalities on the ultrasound even before the ultrasound tech shows any indication of something being off. Unfortunately, this time I was looking at a black mass on the ultrasound screen that I knew should not have been there.
The ultrasound tech could not confirm exactly what the black mass was and said she would show the images to my doctor to review and he would get back to me within the next few days (due to him being out of the office). On the morning of October 15th I did my own Pregnancy and Infant Loss Remembrance Loss Day at home. That was the first time I participated and although it was therapeutic it was also emotionally draining. So imagine how I felt when later that afternoon I got the phone call that there was in fact something off about my ultrasound. My doctor referred to that black mass and said, “It could either be retained products of conception or it could be an indicator of Persistent Gestational Trophoblastic Disease from a partial molar pregnancy. But we should definitely do a second surgery.” In the past I needed two surgeries from one miscarriage to clear my uterus, which was not a big deal other than the inconvenience of a second surgery. But the main difference between that time and this time is that I wasn’t dealing with a partial molar pregnancy before.
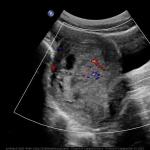
This ultrasound photo is not a picture of my ultrasound, but it appears very similar to what mine looked like with a black mass and cloudy or “snowstorm” appearance surrounding it, typically found with molar pregnancies.

Image Source: MedPix National Library of Medicine
I asked my doctor, “So what’s the next step if this second surgery doesn’t work and it looks like something is still there or develops more?” My doctor told me that I would need to start the medication Methotrexate. His nurse had mentioned that same medication a few days prior when I asked her a similar question. I had assumed that Methotrexate was similar to Misoprostol, which is a common medication I’ve had just prior to each of my surgeries for miscarriages. Misoprostol is a medication softens the uterine lining to make the surgery process easier. I decided to Google what this new medication Methotrexate was, since I was unfamiliar with it. Neither my doctor nor my nurse fully explained what it was. As I was reading the description, all the words fell away except one…chemotherapy. Methotrexate is in fact a type of medication to treat cancer.
My doctor wanted me to have my surgery the following day, but I chose to wait a couple days so I wouldn’t have to take time off work. On Monday (October 21st) I went to my usual surgery center. Out of curiosity I asked my doctor how many times I’ve had surgery there, because I had actually lost count. He looked at my paperwork and told me that this was my fifth surgery there. That did not include the two surgeries I had out-of-state in Seattle for my first and second round of IVF. So in total I’ve had seven surgeries related to infertility and miscarriages from 2016 – 2019.
As of today, October 24th, I’m still waiting for the pathology report to learn what exactly that black mass was. Ultimately this next phone call from my doctor will determine whether I will need chemotherapy or not. I’ve been trying not to worry about it, although the first few days after the 15th were the hardest. I was tossing and turning at night and not getting enough sleep. I told my husband and my Mom. Both of them tried to reassure me by saying “Try not to worry.” But the primary emotion I was feeling was not worry, it was anger.
I was angry at God. I was so angry and frustrated for all of these years of struggling and now He decided to throw in a potential cancer diagnosis. Then my thoughts began to expand out to everyone I’ve known who has battled cancer and how much they suffered. I was thinking, “How could a God allow so much suffering?” God took my Dad away from cancer in 2016 and my mom has survived cancer twice. Then I kept seeing so many commercials on TV for St. Judes Children’s Research Hospital with all those little kids and babies who were completely innocent suffering from cancer. I just could not wrap my mind around any of this.
But I had a conversation with my Mom the other day on the phone that helped me to see things differently. Mind you, I’m not particularly religious. I was “saved” years ago, but after dealing with so much loss over the years my relationship with God was now hanging by a thread. After talking with Mom it helped solidify a thought I had and bring it more to the forefront of my mind. I believe there is a Creator, something greater than us that helped get this world spinning. But as far as a God that intervenes in our daily struggles, well I’ve moved on from that belief.
Believe it or not, I feel more at peace with this concept that God does not intervene. I still believe there is a usefulness to prayer. It can be a way to socially connect on a deeper level and to set positive intentions together. Prayer can also bring us the quiet contemplation we need to help us to potentially find solutions to our problems if we choose to use prayer in that way. What I no longer believe is that praying hard and often leads to the outcome we want. I prayed so hard for each of my babies and set all my intention on positive outcomes. It was suggested to me by various people that perhaps I wasn’t “praying hard enough” or that I needed to “pray more.” I think my issue at the time was my idea of God was changing yet the people around me continued to talk about God the way I used to view Him. These past several years I felt like giving up on my faith. It took me so long to develop a new view of God that He could simply be a Creator and not necessarily an intervener. For me at least this brings me a sense of comfort and peace.
I should be getting my pathology results here soon. I will let you all know what they are once I get them. For now I will be taking it easy resting after this recent surgery. I went back to work the following day after my surgery, which I think was good for me because it serves as a good distraction. I’m trying to take it easy this first week as far as movement goes, by taking a break from exercising. I feel pretty good but have some twinges of pain here and there. I’m going to try to stay optimistic while I wait for my results.
Thank you for reading. 🙂
Today’s Question:
Have your spiritual beliefs changed over time through your infertility struggles? If so, how have they changed?
Comment below with your response to receive a bonus entry to the current contest.
Check out my previous posts by going to my archives page.
This post may contain affiliate links. You can read the disclosure here.
Learn ways to improve your egg quality. Purchase Rebecca Fett’s book “It Starts with the Egg: How the Science of Egg Quality Can Help You Get Pregnant Naturally, Prevent Miscarriage, and Improve Your Odds in IVF.” It’s currently the #1 Best Seller on Amazon.com’s Reproductive Medicine & Technology list.





